Home Stretch | Implants and immune cells
Seize a lizard by its rear end and you are likely to be left holding just a tail. The lizard escapes and its tail simply grows back later. This ability relies on what are called macrophages – immune cells that we humans also possess. PhD candidate Valentina Bonito investigated how we can best use the healing effects of these macrophages to steer the formation of blood vessels or heart valves made of the body's own materials.
At Biomedical Engineering they are studying how the body itself can be prompted to make a new heart valve or (arterial) vein; a field known as in situ tissue engineering. A porous and flexible implant made of biodegradable plastic serves as the basis; nestling in this are the body's own cells, ready to grow into fully functioning tissue.
But this won't happen without a helping hand, says Valentina Bonito. “In principle, any implant like this will be attacked by the immune system; after all it is a foreign body. Playing a vital role in this attack are macrophages, immune cells from the blood stream.” There are two types of these macrophages, she explains. One, referred to by Bonito as M1, which prompts an immune response that results in the forming of scar tissue, and a friendly type, M2, that stimulates the production of new, healthy tissue. In going about their work, however, both these types of immune cell ensure that the implant is dismantled.
“The regenerative process always starts with an inflammatory response caused by cells of the type M1, but at a given moment this response should be halted by macrophages of the M2 type.” The implant needs to interact with the immune cells in such a way that the degradation of the implanted material is kept in balance with the production of new tissue. Otherwise some months down the line the patient will be harboring a heart valve that isn't fully grown or a leaky blood vessel.
Builders
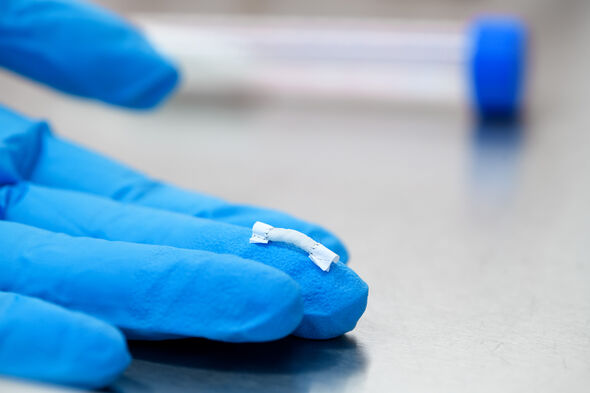
One strategy is to add signal molecules to the implant. These encourage the immune cells to behave in the desired manner: as builders of healthy tissue. Bonito tested this possibility using an implant – a soft, white plastic tube about a centimeter long – that was acting as the aorta in a laboratory rat. “We did indeed see that much more tissue had formed around the implant that we had coated with the molecule interleukin-4, which activates M2 cells. It was amazing to see this three months later, while the role of macrophages tends to be limited to the first few days after implantation.”
But other factors too determine the success of the procedure. Such as the extent to which the cells in the implant are exposed to forces that stretch them, as Bonito saw. The pulsating heart beat causes blood vessels to stretch repeatedly to its rhythm, and that proves to be vitally important to how the macrophages behave and the formation of new tissue. “Moderate forces have proven to deliver the best result. And we can ensure this level of force by using a material that is a little stiffer.”
Personal medicine
For an optimal result, at some future date the influence of other immune cells should also be investigated, the Italian PhD candidate believes. Additionally, this immune response varies - and with it the way in which an implant is received by the body - from person to person, depending on factors such as age, sex and health.
“Consider people with diabetes, a disease that is often accompanied by cardiovascular disorders. They often have more glucose in their blood. You could simulate an environment like this in the lab, in order to learn how it would impact the implants you want to use. With customized treatment for every patient as the ultimate aim.”


Discussion