
Home stretch | Early detection of pregnancy complications
Although most children are born without major complications, problems can arise during pregnancy — often without clear warning signs. New monitoring equipment is generating increasing amounts of data, but the interpretation of that data is lagging behind. To change that, TU/e PhD candidate Ivar de Vries is developing smart algorithms that could help detect complications earlier.
During pregnancy and around birth, complications can arise that affect the health of both mother and child. In perinatal care, four major complications are often grouped together as the so-called “Big 4”: congenital abnormalities, placental problems that restrict fetal growth, preterm birth, and oxygen deprivation during birth. Together, these complications occur in approximately 18% of pregnancies. When babies die after birth or develop serious health problems, this can often be traced back to one of these well-known causes.
At the same time, new technology is now available that can provide far more detailed measurements of fetal condition. “With the new equipment, we don’t just measure the heart rate of the mother and child and uterine activity, but we can also see how contractions spread through the uterus,” explains TU/e researcher Ivar de Vries. However, this additional information remains unused in current clinical practice, because doctors are not yet sure how to interpret the data.
That is exactly the focus of Ivar de Vries’ PhD research. He is developing practical tools for medical professionals: how can these new measurements be used to detect complications earlier and more accurately?
During his PhD, he carried out dozens of measurements at Máxima MC and worked on algorithms that extract meaningful information from the data. The goal is to improve diagnostics for all four main causes, enabling doctors to intervene earlier and give babies a better chance.
Improving survival rates
“Right now, the problem is that doctors still don’t have a clear enough picture of who needs treatment,” De Vries explains. Risk factors are known, but they do not always lead to accurate assessments. As a result, pregnant women are sometimes treated or admitted to hospital unnecessarily—in cases of threatened preterm birth, this applies to about half of all cases.
At the same time, patients who are actually at risk sometimes go unnoticed. “When things go wrong, it is not always recognized in time, even though early intervention can significantly improve a baby’s chances of survival,” De Vries emphasizes.
“For the first time, we are able to collect this type of data, so it’s a unique opportunity to extract something valuable from it,” he says. “By comparing data from healthy and high-risk pregnancies, we can translate new medical technology into something that is truly useful in clinical practice.”
The human side of data
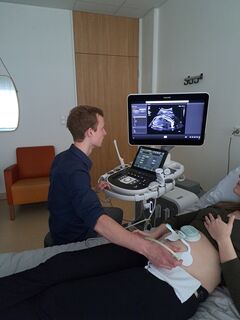
To better understand the needs of medical staff and align his research accordingly, De Vries worked full-time in the hospital during his PhD. He collected data during ultrasounds and was even present at several cesarean sections. This not only gave him a unique insight into clinical practice, but also brought him into contact with patients—an experience he describes as particularly meaningful.
“You speak with people who have experienced things going wrong during pregnancy. The questions and uncertainties they had show what they actually need help with. That gives direction to your research. Those conversations are also very motivating, because you really see the human behind all the data and understand what you are doing it for.”
He also values working side by side with doctors. “At the beginning, I was missing that medical background, so it was very helpful to sit at the same desk and work together,” De Vries says. The collaboration between medical and technical expertise worked extremely well, he adds. “Quite a few research ideas were born at the coffee machine.”
Preterm birth
In nearly half of babies who die after birth, preterm birth is the cause. Medication can be given to help the baby’s lungs mature, but it must be administered 48 hours in advance and only works for about seven days. “This medication also has side effects, so you only want to give it when it is truly necessary—and not more than twice,” De Vries explains.
With one of the algorithms he developed, it is now possible not only to predict preterm birth, but also to estimate when delivery will occur. This allows medication to be given in time, and only to women who truly need it. At the same time, women without elevated risk can stay at home, avoiding the stress of unnecessary hospital admission.
A heart tracing without noise
Another complication De Vries focuses on is congenital abnormalities. These occur when organs or structures in the fetus do not develop properly. When the heart is affected—the most critical organ—this can be life-threatening. In the Netherlands, early ultrasounds are already performed, yet around 40 percent of heart defects are still missed.
“With the new equipment, we can create a heart tracing of the baby,” De Vries explains. “But because the baby is in the uterus, behind the mother’s abdominal muscles, there is a lot of noise. With a specially developed algorithm, we can largely remove that noise, giving us a much clearer signal.”
Another algorithm can then determine, based on the heart tracing, whether a congenital heart defect is present. “Otherwise, you would have to train all gynecologists to interpret this data—they are not cardiologists, after all.” The system can automatically flag high-risk cases, which can then be sent to an expert center for further evaluation.
Acting quickly
With the new technology, it may become possible to detect more abnormalities early on. Not all babies can be saved, but with early detection, pregnant women still have time to consider terminating the pregnancy. For many, this is less traumatic than continuing a pregnancy knowing the child will likely die shortly after birth.
In some cases, a newborn can be operated on immediately after delivery. In those situations, it is essential that the condition is known in advance, so the medical team can prepare and act quickly.
Placenta
Problems with the placenta can lead to preeclampsia, a condition that can also be dangerous for the mother. It causes high blood pressure, which in severe cases can lead to kidney or heart failure, and even death. “At the moment, we cannot predict preeclampsia. And once kidney failure has occurred, you are essentially too late,” De Vries explains.
From new measurements, however, De Vries has been able to identify important biomarkers that can predict preeclampsia early in pregnancy—weeks before the condition develops. This allows doctors to monitor pregnant women at increased risk more closely.
Practical applications
“The diagnostic methods still need to be validated, but in principle the technology is almost ready to be used in hospitals,” the PhD candidate says hopefully. The fact that the research has so many practical applications is directly linked to its starting point: it was driven by the questions and needs of gynecologists. “We’ve created something they can actually use—and that works.”
That need is also urgent. “Gynecologists are sometimes still left empty-handed, so anything they can use is seized with both hands.” The goal is for the methods to quickly find their way into clinical practice, so that both unborn and born babies have better chances.
PhD in the picture
What is on the cover of your dissertation?
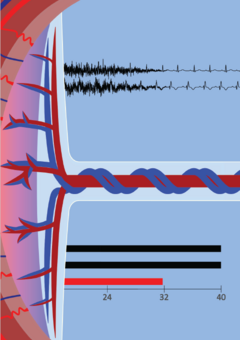
“I tried to represent the four major complications. You see a placenta transitioning into an umbilical cord, a timeline pointing to preterm birth, and a heart tracing.”
How would you explain your research at a birthday party in one sentence?
“I study new methods to detect problems during pregnancy earlier.”
How do you blow off steam outside the lab?
“I do a lot of running and I’m training for a half marathon. I’m also involved in scouting, where I volunteer as a group leader for children aged seven to ten. I really enjoy doing that.”
What advice would you have given yourself as a starting PhD candidate?
“It was a very good decision to collect my own data in the hospital and to work closely with doctors. Interdisciplinary collaboration has really been the strength of my research. It allowed us to help each other whenever we got stuck: they with an Excel sheet, and I for example with medical literature.”
What’s your next chapter?
“I will continue this research as a postdoc. I want to carry on with the work I did during my PhD. The next step is to further develop it into a product that allows us to conduct clinical studies and ultimately have something that can truly be applied in practice.”

Discussion